Protecting Your Child From Dehydration and Heat Illness
1. What puts my child at risk for dehydration?
The same things that put you at risk for dehydration: prolonged exposure to high temperatures, direct sun, and high humidity, without sufficient rest and fluids. The difference is that a child’s body surface area makes up a much greater proportion of his overall weight than an adult’s, which means children face a much greater risk of dehydration and heat-related illness.
2. What signs of dehydration should we watch for?
Early signs of dehydration include fatigue, thirst, dry lips and tongue, lack of energy, and feeling overheated. But if kids wait to drink until they feel thirsty, they’re already dehydrated. Thirst doesn’t really kick in until a child has lost 2% of his or her body weight as sweat.
Untreated dehydration can lead to three worse types of heat illness:
- Heat cramps: Painful cramps of the abdominal muscles, arms, or legs.
- Heat exhaustion: Dizziness, nausea, vomiting, headaches, weakness, muscle pain, and sometimes unconsciousness.
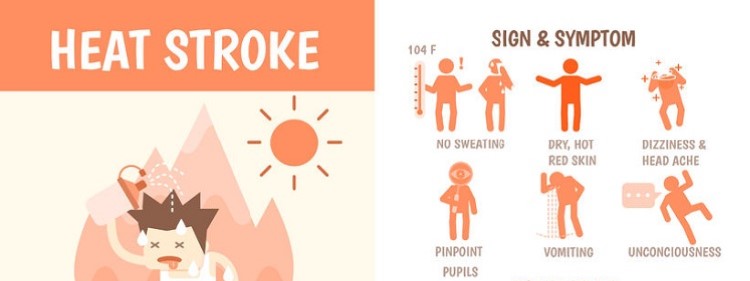
- Heat stroke: A temperature of 104 F or higher and severe symptoms, including nausea and vomiting, seizures, disorientation or delirium, lack of sweating, shortness of breath, unconsciousness, and coma.
Both heat exhaustion and heat stroke require immediate care. Heat strokeis a medical emergency that, when untreated, can be deadly. Any child with heat stroke should be rushed to the nearest hospital.
3. What can I do to prevent dehydration in my child?
Make sure they drink cool water early and often. Send your child out to practice or play fully hydrated. Then, during play, make sure your child takes regular breaks to drink fluid, even if your child isn’t thirsty. A good size drink for a child, according to the American Academy of Pediatrics, is 5 ounces of cold tap water for a child weighing 88 pounds, and nine ounces for a teen weighing 132 pounds. One ounce is about two kid-size gulps.
Get them acclimatized before summer practice. “If you’re going to send your kid off to tennis camp, they shouldn’t be sitting around doing nothing in May and then going out to play tennis eight hours a day in June,” says Hergenroeder. “They should be outdoors jogging, riding a bike, and otherwise slowly building up their fitness and ability to handle the heat.” The fitter children are, the sooner their bodies will start to sweat after beginning to exercise — and that’s a good thing!
Know that dehydration is cumulative. If your child is 1% or 2% dehydrated on Monday and doesn’t drink enough fluids that night, then gets 1% or 2% dehydrated again on Tuesday, that means your child is 3% or 4% dehydrated at the end of the day. “They may be gradually developing a problem, but it won’t show up for several days,” says Hergenroeder. “You should always monitor your child’s hydration.” One way to do this: weigh your child before and after practice. If his weight drops, he’s not drinking enough during his workout.
A simple rule of thumb: if your child’s urine is dark in color, rather than clear or light yellow, he or she may be becoming dehydrated.
4. If my child develops heat illness, what can I do to treat it?
The first thing you should do with any heat illness is get the child out of the sun into a cool, comfortable place. Have the child start drinking plenty of cool fluids. The child should also take off any excess layers of clothing or bulky equipment. You can put cool, wet cloths on overheated skin. In cases of heat cramps, gentle stretches to the affected muscle should relieve the pain.
Kids with heat exhaustion should be treated in the same way but should not be allowed back on the field the same day. Monitor your child even more carefully, Hergenroeder says. If your child doesn’t improve, or can’t take fluids, see a doctor.
Heat stroke is always an emergency and requires immediate medical attention.
5. Are some children more prone to dehydration or heat illness than others?
Yes, says Hergenroeder. One of the biggest risk factors: a previous episode of dehydration or heat illness. Other factors that can put your child at greater risk for heat illness include obesity, recent illness (especially if the child has been vomiting or has had diarrhea), and use of antihistamines or diuretics.
Lack of acclimatization to hot weather and exercising beyond their level of fitness can also lead to heat illness in young athletes. “If a young player isn’t in shape and tries to go out and do things quickly to ‘make the team’ — or goes to summer practice or summer camp and hasn’t been used to that kind of heat and humidity and duration of exercise — that sets them up for dehydration and heat illness,” Hergenroeder says.
6. Is it ever too hot for my child to practice or play sports?
A growing number of athletic programs suggest that it is sometimes too hot to practice. In fact, many are restricting outdoor practice when the National Weather Service’s heat index rises above a certain temperature. The heat index, measured in degrees Fahrenheit, is an accurate measure of how hot it really feels when the relative humidity is added to the actual temperature.
The National Athletic Trainers’ Association (NATA) offers information and guidelines for parents and coaches on their web site.
WebMD Medical Reference Reviewed by Renee A. Alli, MD on August 11, 2017